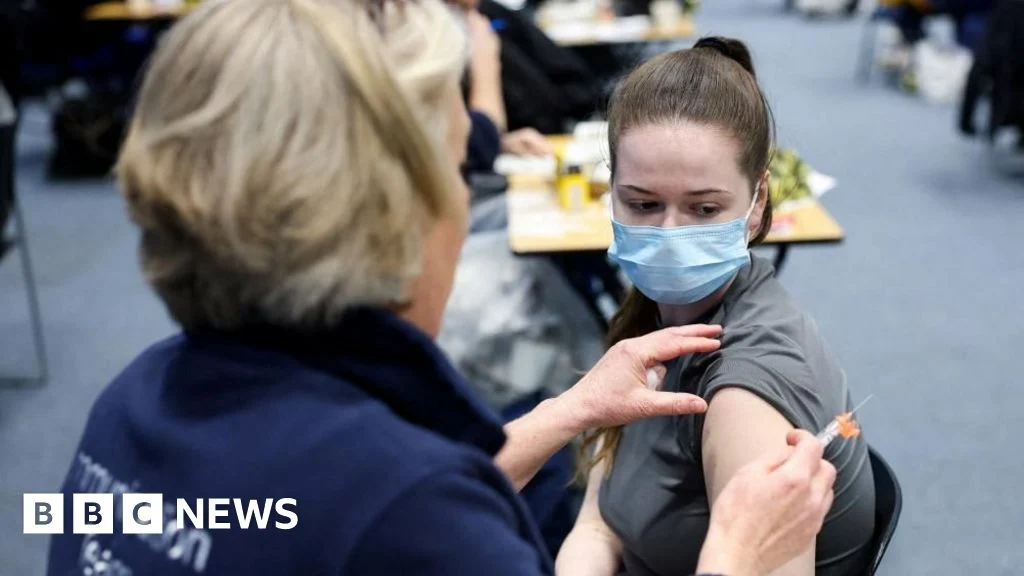
In a significant public health intervention, the UK Health Security Agency (UKHSA) has announced the expansion of its Meningitis B vaccination programme to include Year 11 pupils in specific Kent schools, broadening the protective shield against a recent localized outbreak. This precautionary measure aims to bolster community immunity among 15 and 16-year-olds, ensuring sustained defence in areas where older students have already received their doses. The decision comes amidst intensive efforts to contain the spread of the bacterial infection, which has seen a concentrated cluster of cases predominantly affecting young adults in the region.
Meningitis B, caused by the bacterium Neisseria meningitidis group B, is a severe and potentially life-threatening infection that can lead to meningitis (inflammation of the membranes surrounding the brain and spinal cord) and septicaemia (blood poisoning). The disease can progress rapidly, often manifesting initially with non-specific symptoms such as fever, headache, vomiting, and muscle pain, making early diagnosis challenging. Characteristic symptoms like a non-blanching rash, stiff neck, and sensitivity to light typically appear later in the disease progression. Young people, particularly those in close living quarters such as schools and universities, are considered a higher-risk group due to increased social interaction and potential for transmission. The rapid onset and severe consequences, including permanent neurological damage, limb loss, or even death, underscore the critical importance of swift public health responses and preventative vaccination.
The current outbreak in Kent has prompted an urgent and robust response from health authorities. According to the latest figures from the UKHSA, the number of confirmed Meningitis B cases remains at 20, with an additional three cases still under thorough investigation. This represents a reduction from the 29 total cases initially reported, indicating a degree of stabilization, although vigilance remains paramount. The vast majority of those affected are young individuals, with an average age of 19, highlighting the demographic vulnerability that necessitated the targeted vaccination strategy. Disturbingly, four individuals who contracted the infection were still receiving intensive care as of Monday, underscoring the severe nature of the disease and the critical condition of some patients.
Tracing the timeline of the outbreak, the UKHSA’s report on Tuesday pinpointed the earliest identified case to March 9, with the most recent case occurring on March 16. The peak incidence of the outbreak was observed on March 13, indicating a concentrated period of transmission within a short timeframe. This rapid clustering of cases prompted the immediate activation of extensive public health protocols, including contact tracing, prophylactic antibiotic administration, and the implementation of mass vaccination clinics. To date, over 10,000 Meningitis B vaccine doses have been administered as part of this focused intervention, alongside more than 13,000 doses of antibiotics provided to close contacts to mitigate potential further spread.
The decision to extend vaccination to Year 11 pupils is a strategic enhancement of the existing containment efforts. By vaccinating 15 and 16-year-olds in schools where older students have already been inoculated, the UKHSA aims to create a more comprehensive protective barrier across susceptible age groups within affected educational environments. This forward-looking approach seeks to prevent future infections and establish longer-term immunity, especially as these students transition through various social settings. The logistical challenge of delivering such a large-scale vaccination and antibiotic distribution programme within a short timeframe has been substantial, requiring significant coordination between health services, local authorities, and educational institutions.
A crucial aspect of the UKHSA’s response has been the rapid scientific analysis of the specific strain of Meningitis B responsible for the Kent outbreak. Professor Robin May, Chief Scientific Officer at the UKHSA, provided a reassuring assessment, stating that detailed laboratory analysis offers "strong reassurance that our existing vaccinations and antibiotic treatment offer will be effective against this strain." This confirmation is vital, as bacterial strains can sometimes exhibit variations that impact the efficacy of standard treatments or vaccines. The ability to confirm the susceptibility of the outbreak strain to current medical interventions significantly strengthens the public health response and instills confidence in the chosen strategy.
The UKHSA report also acknowledged that several factors could be contributing to the observed outbreak patterns. These include potential differences in the specific bacterial strain circulating, varying levels of natural or vaccine-induced immunity within the population, and a confluence of social and environmental factors that facilitate transmission. Congregate settings, such as schools and colleges, inherently pose a higher risk for infectious disease spread due to close contact among individuals. Environmental factors, such as seasonal variations in respiratory illnesses that can predispose individuals to bacterial infections, may also play a role. Understanding these multifactorial dynamics is crucial for developing targeted and effective public health interventions.
Beyond the immediate crisis management, the Kent Meningitis B outbreak carries broader implications for public health policy and disease surveillance. It underscores the continuous need for robust epidemiological monitoring systems capable of detecting unusual clusters of infectious diseases rapidly. The swift identification of this outbreak and the subsequent deployment of comprehensive vaccination and treatment programmes demonstrate the critical capacity of the UK’s public health infrastructure to respond to acute threats. The experience gained from managing this localized emergency will undoubtedly inform future strategies for preventing and controlling similar outbreaks.
The proactive vaccination of a broader age cohort serves not only to protect individuals but also to reduce the overall burden of the disease within the community by limiting its potential for wider dissemination. While routine Meningitis B vaccination is offered to infants and, more recently, to adolescents in specific catch-up programmes, localized outbreaks necessitate flexible and responsive adjustments to these schedules. This incident highlights the dynamic nature of infectious disease threats and the importance of adapting public health measures to evolving circumstances.
Looking ahead, ongoing surveillance will be critical to monitor the effectiveness of the vaccination campaign and to detect any further cases or shifts in the outbreak’s trajectory. Public awareness campaigns regarding the symptoms of Meningitis B and the importance of seeking urgent medical attention remain essential, particularly for parents and young people. Furthermore, continued research into meningococcal disease epidemiology, vaccine development, and antibiotic resistance patterns will be vital in strengthening global preparedness against future outbreaks. The coordinated effort in Kent serves as a testament to the dedication of health professionals and the efficacy of structured public health interventions in safeguarding community well-being against severe infectious diseases.






