Authorities in North London have initiated a stringent public health measure, informing parents that unvaccinated children identified as close contacts in the burgeoning measles outbreak could face temporary exclusion from educational institutions. This decisive action underscores the increasing concern among health officials regarding the highly transmissible disease, as vaccination rates in parts of the capital fall perilously below the critical threshold required for community protection.
The directive, communicated to parents across boroughs such as Enfield and Haringey, mandates that pupils without full measles, mumps, and rubella (MMR) vaccination may be excluded from schools for a period of 21 days following exposure to a confirmed case. This period aligns with the typical incubation timeline for measles, aiming to curtail further transmission within school environments. Local health leaders have expressed profound apprehension, noting that the current surge in cases represents a significant deviation from typical epidemiological patterns observed in the region. The confirmation of infections across at least seven schools and nurseries within these neighbouring boroughs highlights the rapid and widespread nature of the current viral activity.
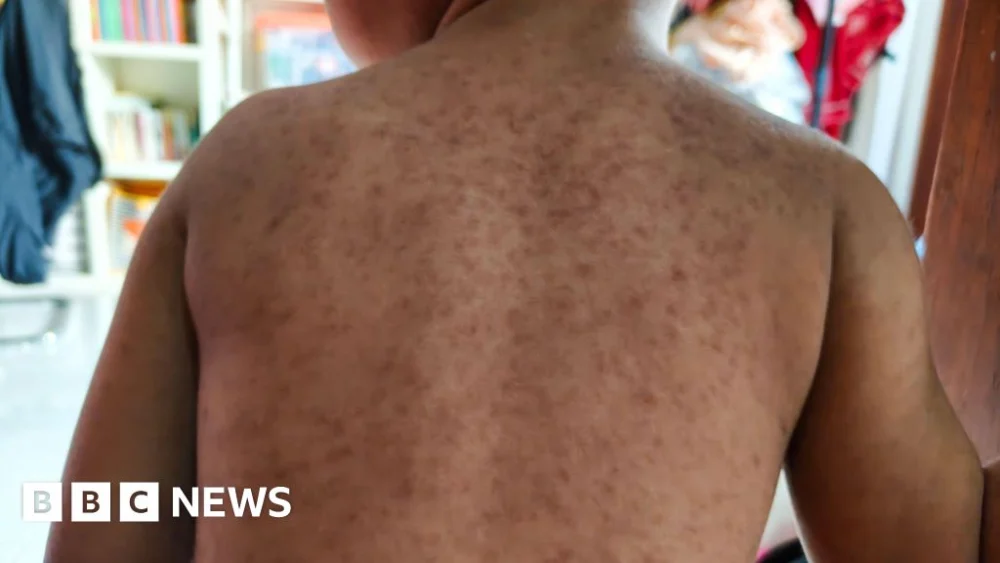
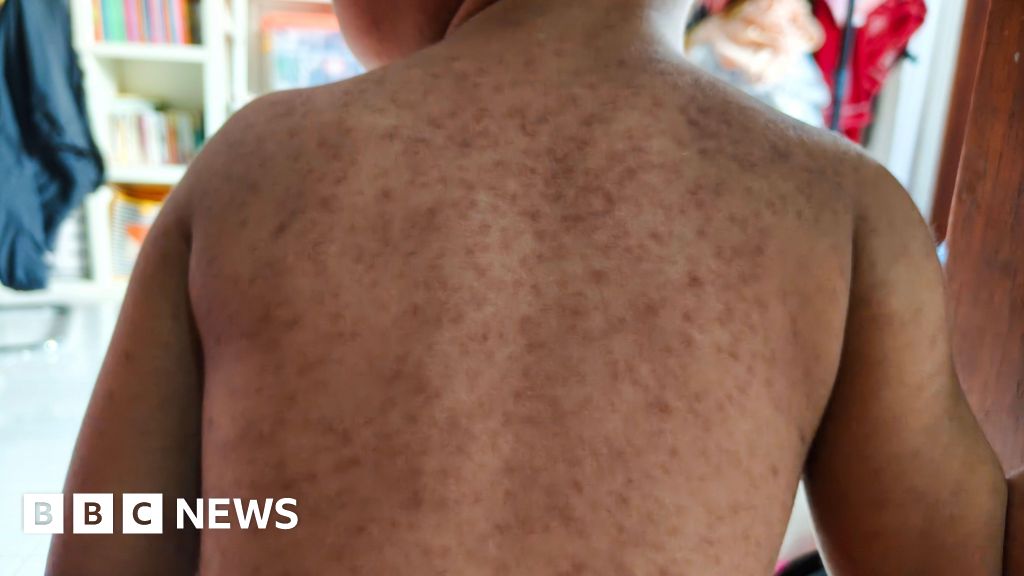
Measles, often underestimated due to its historical decline, is far more than a childhood inconvenience. It is a severe, potentially life-threatening viral illness. Initial symptoms typically manifest as a high fever, persistent cough, runny nose, and red, watery eyes. These are often followed by the characteristic measles rash, which generally begins behind the ears and on the face before spreading across the body. Crucially, on darker skin tones, this rash can be more challenging to detect, appearing as subtle changes in texture or a muted discoloration rather than the vivid red seen on lighter complexions. A distinctive diagnostic feature, though not always present, is the appearance of tiny white spots, known as Koplik’s spots, inside the mouth.
The disease’s high contagiousness is a primary driver of public health concern. The measles virus spreads through airborne droplets released when an infected person coughs or sneezes. These droplets can remain viable in the air for up to two hours after the infected individual has left the area, meaning transmission can occur without direct contact. Its basic reproduction number (R0) is estimated to be between 12 and 18 in susceptible populations, making it one of the most infectious human diseases known. This necessitates extremely high vaccination coverage to achieve herd immunity, thereby protecting those who cannot be vaccinated, such as infants, pregnant women, and individuals with compromised immune systems.
The potential complications of measles are severe and warrant serious attention. While many cases resolve without major issues, a significant proportion can lead to serious health problems. These include pneumonia, a leading cause of measles-related deaths in young children, and encephalitis, an inflammation of the brain that can result in permanent brain damage, deafness, or intellectual disability. Other complications encompass ear infections, severe diarrhoea, and, in rare but devastating instances, subacute sclerosing panencephalitis (SSPE), a fatal neurological disorder that can develop years after the initial infection. The risk of these complications is notably elevated in infants, malnourished children, and individuals with weakened immune systems, underscoring the vital protective role of widespread vaccination.
The public health measure of excluding unvaccinated close contacts from schools is not unprecedented; it is a standard protocol deployed in many jurisdictions during outbreaks of highly contagious diseases. This strategy is predicated on the understanding of viral transmission dynamics and the incubation period. By removing potentially infected but asymptomatic individuals from environments with high concentrations of susceptible persons, such as schools, the chain of transmission can be effectively broken. The 21-day exclusion period accounts for the maximum incubation time of measles, ensuring that by the time a child returns to school, they would either have developed symptoms (and thus be identified and isolated) or would have passed the infectious stage without developing the disease. This policy, while disruptive for families, is a critical tool for outbreak containment, balancing individual educational access against the imperative of community health protection.
This local crisis unfolds against a backdrop of deteriorating national measles immunity. The United Kingdom recently lost its World Health Organization (WHO) "measles elimination status," a significant setback indicating that the disease is once again endemic within the country, rather than being imported and contained. This status is conferred when a country demonstrates the absence of continuous measles transmission for at least three consecutive years, supported by a robust surveillance system. The recent re-establishment of endemic transmission signifies a failure to maintain sufficiently high vaccination rates, leaving communities vulnerable to widespread outbreaks. Epidemiological data confirms this alarming trend, with thousands of measles cases reported across England in recent years, reaching levels not seen in over a decade. This resurgence stands in stark contrast to the near eradication of measles in developed nations just a few decades ago, a testament to the success of comprehensive vaccination programmes.
The decline in MMR vaccination uptake is a multifaceted issue, reflecting a complex interplay of systemic, social, and individual factors. In Enfield, for instance, only 64.3% of five-year-olds had received both recommended doses of the MMR vaccine in the latest reporting period. This figure is dramatically lower than the 95% threshold universally recognized as necessary to achieve effective herd immunity and prevent outbreaks. Nationally, the uptake rate has also fallen, dropping from a peak of nearly 89% a decade ago to just over 84% currently.
Several contributing factors have been identified by health experts. One significant barrier relates to accessibility and convenience, with many parents reportedly struggling to secure timely appointments for their children’s vaccinations. This can be exacerbated by pressures on primary care services, including staffing shortages and reduced availability of dedicated immunization clinics. Compounding this is a widespread lack of awareness regarding the severity of measles. For generations, the disease was largely absent due to high vaccination rates, leading to a diminished collective memory of its devastating potential. This complacency can result in a lower perceived urgency for vaccination.
Furthermore, concerns surrounding vaccine safety, though often rooted in debunked scientific claims, continue to fuel vaccine hesitancy. While outright "vaccine refusers" who actively oppose all vaccinations constitute a minority, a larger segment of the population falls into the category of "vaccine hesitant." These individuals may have legitimate questions, seek more information, or express distrust in health authorities, often influenced by the proliferation of misinformation and conspiracy theories on social media platforms. The COVID-19 pandemic also played a role, disrupting routine immunization schedules and potentially diverting public attention and resources away from other essential health services, including childhood vaccinations.
Healthcare professionals are pivotal in reversing this concerning trend. Local general practitioners, like Dr. Ellie Cannon in North London, highlight the rarity of measles cases in their professional careers, emphasizing the significant shift the current outbreak represents. This generational gap in experience means that many younger clinicians may not have personally witnessed the severe complications of measles, underscoring the need for continuous education and awareness within the medical community itself.
The strategy for improving vaccination rates must be multifaceted and community-centric. Direct engagement with families is crucial, allowing healthcare providers to empathetically address parental concerns, clarify misconceptions, and unequivocally emphasize the safety and efficacy of the MMR vaccine. This requires dedicated time for consultations, providing accurate, evidence-based information, and building trust. Public health campaigns need to be reinvigorated, not only to raise awareness about the availability of vaccines but also to vividly communicate the real risks and consequences of measles infection, particularly for vulnerable populations. Mobile vaccination clinics, school-based immunization drives, and outreach programmes targeting underserved communities could also play a vital role in enhancing accessibility and overcoming practical barriers.
The long-term implications of declining vaccination rates and sustained measles outbreaks are considerable. Beyond the immediate health burden on affected individuals and the healthcare system, there are significant societal costs. The economic strain on health services, encompassing hospitalizations, intensive care, and extensive public health efforts for outbreak control, is substantial. Educational continuity is also severely disrupted for excluded children, potentially impacting their learning and development. If current trends persist, the UK risks becoming a persistent hotspot for measles, posing a continuous threat to public health and eroding the hard-won achievements of past immunization efforts.
Addressing the current measles crisis in North London and the broader national decline in MMR vaccination uptake demands urgent, concerted action. This includes reinforcing public health communication strategies, enhancing accessibility to vaccination services, and fostering a renewed understanding of the critical importance of collective immunity. The re-establishment of robust vaccination coverage is not merely a matter of individual choice but a collective responsibility essential for safeguarding the health and well-being of the entire community, particularly its most vulnerable members.






