A concentrated public health effort in Kent appears to be yielding positive results, with a notable reduction in the reported incidence of meningitis following a recent localized outbreak that tragically claimed the lives of two young individuals. The UK Health Security Agency (UKHSA) has indicated a decline in confirmed and suspected cases, reflecting the robust and coordinated response by health authorities and local partners to contain the potentially devastating bacterial infection. This shift signals cautious optimism amidst a period of heightened vigilance and underscores the critical importance of rapid diagnostic processes and targeted preventative measures in mitigating infectious disease spread within vulnerable communities.
The initial days of the outbreak were marked by a concerning rise in reported cases, culminating in 34 individuals either confirmed or suspected of having contracted the illness. However, the most recent data released by the UKHSA reveals a decrease to 29 cases, a reduction attributed, in part, to the rigorous reclassification process where initial suspected diagnoses were either ruled out or downgraded following comprehensive laboratory testing. This meticulous verification is a standard and essential component of outbreak management, ensuring that resources are precisely allocated and public anxiety is managed with accurate information. The geographical and demographic focus of this cluster has been predominantly among young people, particularly students, in the Canterbury area, a demographic known to be at elevated risk due to close living quarters and social interactions.
The gravity of the situation was underscored by two tragic fatalities last weekend: Juliette Kenny, a sixth-form student from Queen Elizabeth’s Grammar School in Faversham, and an unnamed student from the University of Kent. These losses served as a stark reminder of the rapid and severe progression that bacterial meningitis, particularly the Meningitis B strain implicated in this outbreak, can inflict. The disease, an inflammation of the membranes surrounding the brain and spinal cord, demands immediate medical attention due to its potential for swift deterioration and severe complications, including brain damage, hearing loss, limb amputation, or death. Its initial symptoms can be deceptively non-specific, often mimicking common viral illnesses, making early diagnosis challenging but paramount. Typical manifestations include a sudden fever, severe headache, stiff neck, confusion, sensitivity to light (photophobia), and a distinctive rash that does not fade under pressure.
The scope of the outbreak extended across multiple educational institutions, with a recent suspected case at EKC Canterbury College adding to the list of affected sites. This brought the total number of educational settings with confirmed or suspected cases to six, including Norton Knatchbull School in Ashford, Simon Langton Grammar School for Boys, and The Canterbury Academy, alongside the aforementioned University of Kent. This pattern of spread within academic environments highlights the epidemiological challenges posed by such infections in settings where close contact is frequent. Dr. Anjan Ghosh, Director of Public Health at Kent County Council, provided further granularity, confirming 20 cases and categorizing nine as probable. Of the confirmed cases, 16 were university students, and four were secondary school pupils, reinforcing the demographic vulnerability observed.
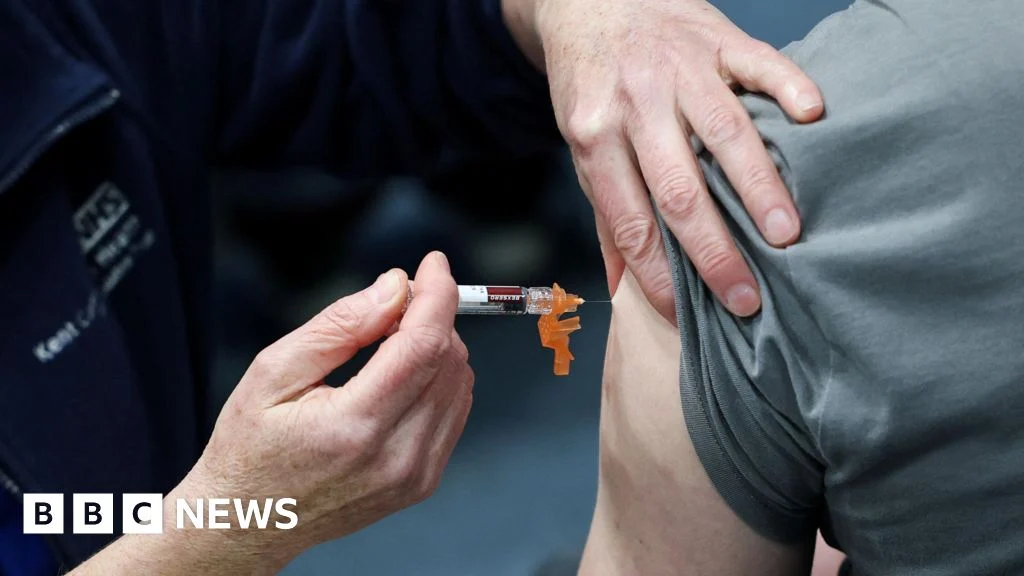
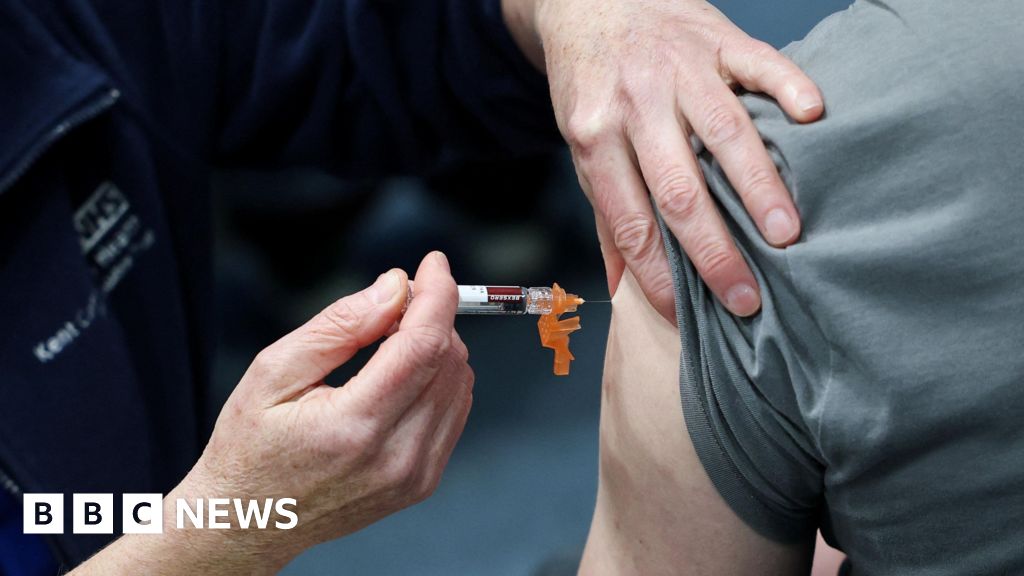
In response to the evolving situation, the UKHSA, in close collaboration with NHS England and local health authorities, has implemented a multi-pronged strategy. Dr. Sherine Thomas, a key figure in the response, affirmed the agency’s "vigilance" and commitment to swift action should any new cases emerge. This proactive stance is crucial for limiting further transmission. A central pillar of the immediate public health response has been the targeted administration of preventative antibiotics to close contacts of infected individuals. This measure, aimed at eradicating the bacteria from carriers before symptoms can develop, has seen over 12,150 people receive prophylactic treatment. Concurrently, a focused Meningitis B (MenB) vaccination program has been rolled out, reaching more than 8,000 individuals. While antibiotics offer immediate protection, the MenB vaccination provides the most effective long-term immunity against the specific strain circulating. This dual approach exemplifies the comprehensive strategy required to manage bacterial outbreaks effectively.
A significant factor contributing to the vulnerability of the affected age group is the historical timeline of MenB vaccination. Routine immunization against Meningitis B was introduced into the national schedule for infants in the UK in 2015. Consequently, the current cohort of university and secondary school students, typically in their late teens or early twenties, generally falls outside the age groups routinely vaccinated as children. This gap in protection leaves a substantial portion of the young adult population susceptible, a critical consideration that has prompted calls for a review of vaccine policy. Health Secretary Wes Streeting has publicly stated his intention to seek advice from the Joint Committee on Vaccination and Immunisation (JCVI) regarding the potential expansion of MenB vaccine availability to older age groups. Such a review would involve a thorough assessment of the epidemiological burden, vaccine efficacy in different age cohorts, and the cost-effectiveness of a broader immunization program.
Beyond the immediate medical response, the outbreak has had tangible effects on the wider community. Businesses in Canterbury have reported a noticeable decrease in patronage, with some lamenting that students, gripped by concern, are "hiding in their bedrooms." This anecdotal evidence points to the broader societal and economic ripple effects that even localized infectious disease outbreaks can generate, impacting local economies and fostering a climate of apprehension. The psychological toll on students and their families has also been significant, as exemplified by a University of Kent student who made a pre-dawn drive from Ipswich with his mother to secure a vaccine, highlighting the palpable anxiety and proactive measures individuals are taking to protect themselves.
Amidst the public concern, expert reassurances have been critical. Professor Shamez Ladhani from the UKHSA has expressed confidence in the containment efforts, emphasizing that the bacterium responsible for meningitis does not spread with the same ease as highly contagious respiratory viruses like influenza or COVID-19. He clarified that the risk to the general public remains at a "baseline," as transmission typically requires prolonged, close contact, such as through kissing or living in the same household, rather than casual encounters. This distinction is vital for tempering public fear and ensuring that appropriate, rather than excessive, precautions are taken. Health Secretary Streeting further underscored this message, urging the public to "keep living your lives, and keep looking after one another," while strictly adhering to medical advice. He also extended commendation for the "Herculean efforts" of frontline healthcare workers and public health professionals who have tirelessly managed the crisis.

The Kent meningitis outbreak serves as a poignant case study in modern public health challenges, illustrating the dynamic interplay between disease epidemiology, targeted intervention strategies, and effective public communication. The ongoing decline in cases, coupled with the rigorous identification and management of contacts, suggests that the immediate threat is being effectively managed. However, the broader implications extend to future vaccine policy, particularly for vulnerable age cohorts, and the continuous need for robust surveillance systems. The commitment to reviewing vaccination guidelines by the JCVI could lead to a significant re-evaluation of national immunization programs, potentially expanding protection to more age groups and thereby fortifying public health resilience against future outbreaks of this severe disease. The lessons learned from Canterbury will undoubtedly inform and strengthen infectious disease control strategies across the nation, emphasizing preparedness, rapid response, and community engagement as cornerstones of public health security.