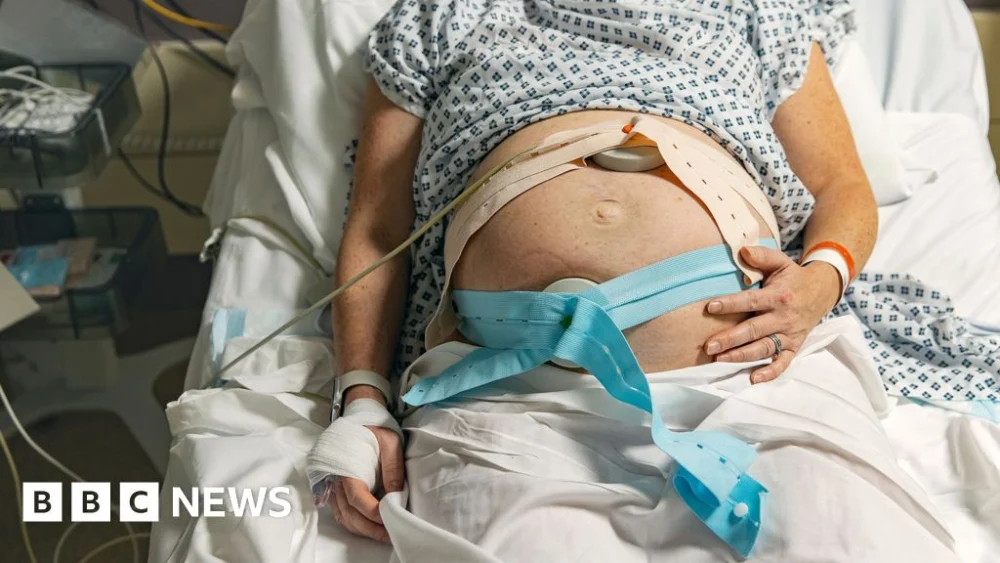
A comprehensive interim assessment has brought to light profound and pervasive shortcomings within England’s maternity and neonatal care landscape, indicating widespread systemic failures that impact families throughout the entire continuum of obstetric and postnatal support. The preliminary findings of a government-commissioned review, led by Baroness Amos, delineate a troubling picture where critical issues such as institutional racism, severe staffing shortages, and a pervasive lack of accountability are contributing to suboptimal and, at times, dangerous outcomes for mothers and infants. This interim report, drawing upon extensive evidence from thousands of individuals, underscores a deeply inconsistent quality of care that ranges from exemplary to severely deficient, prompting urgent calls for fundamental reform.
Baroness Amos’s independent review, initiated to thoroughly investigate the state of maternity and neonatal services across England, has already gathered submissions from over 8,000 individuals and engaged in direct consultations with more than 400 families affected by care provision. Her initial conclusions, articulated during a recent broadcast interview, highlight a troubling dichotomy: while instances of safe and excellent care exist, these are frequently overshadowed by "way too many examples of poor care." This inconsistent delivery, described as "patchy" and "inconsistent," points to deep-seated issues rather than isolated incidents, suggesting a systemic vulnerability within the National Health Service (NHS) trusts responsible for these vital services. The final recommendations of the review are anticipated in April, with Health Secretary Wes Streeting having committed to acting upon them.
The interim report identifies six critical areas of concern, though the specific details of all six were not fully enumerated in the initial public statements. However, the prominent mention of racism, staffing challenges, and accountability issues provides a clear indication of the review’s central focus.
The Pervasive Impact of Racism in Maternity Care
The explicit identification of racism as a significant factor in maternity care failings represents a crucial, albeit disturbing, finding. This speaks to long-standing concerns voiced by Black, Asian, and minority ethnic (BAME) communities regarding disparities in healthcare access, treatment, and outcomes. Systemic racism in healthcare can manifest in various forms, including unconscious bias among staff, discriminatory practices in communication and decision-making, and a failure to adequately address the specific needs and cultural contexts of diverse patient populations.
The consequences of such discrimination are often dire. Studies and anecdotal evidence have consistently shown that BAME women in England face higher rates of maternal mortality and morbidity compared to their white counterparts. This disparity is not solely attributable to socioeconomic factors but is intrinsically linked to how these women are perceived, listened to, and treated within clinical environments. Instances of pain being dismissed, concerns being overlooked, and a general lack of empathy or understanding contribute to a diminished standard of care, increasing risks during what is already a vulnerable period. Addressing this requires not only policy changes but a profound cultural shift within healthcare institutions, mandating comprehensive anti-racism training, equitable workforce representation, and robust mechanisms for reporting and investigating discriminatory incidents.
Critical Understaffing and its Ripple Effects
The report’s emphasis on staffing issues as a major contributor to care failings underscores a chronic problem plaguing the NHS. Insufficient numbers of midwives, obstetricians, and support staff lead directly to increased workloads, burnout, and a reduced capacity for delivering personalized and safe care. When services are understaffed, continuity of care often suffers, meaning mothers may see different professionals at various stages of their pregnancy and labour, hindering the development of trust and comprehensive understanding of their individual needs.
Furthermore, staffing shortages compromise the ability of units to respond effectively to emergencies, increase the likelihood of errors, and reduce the time available for crucial communication with families. The relentless pressure on existing staff can also lead to a decline in morale and a greater propensity for staff to leave the profession, exacerbating the cycle of understaffing. Addressing this requires strategic long-term workforce planning, significant investment in recruitment and retention initiatives, and creating supportive working environments that prioritize staff well-being and professional development. Without an adequately staffed and well-supported workforce, efforts to improve the quality and safety of maternity care will remain severely hampered.
A Deficit in Accountability and Learning
The third significant factor highlighted by Baroness Amos is the issue of accountability. A lack of clear and effective accountability mechanisms can create an environment where poor practices persist, errors are not adequately investigated, and lessons are not learned. This can manifest as a failure to take responsibility for mistakes, an absence of transparent reporting, and insufficient consequences for negligence. When healthcare professionals or institutions are not held accountable for failings, it erodes trust, impedes systemic improvement, and perpetuates a culture where preventable harm can continue.
The report implicitly points to a cultural problem where, as some families suggest, the professional expertise of midwives or doctors is sometimes prioritised over the lived experience and concerns of the birthing mother. This "not listening" culture, as described by affected families, represents a critical breakdown in patient-centred care. Effective accountability frameworks must encompass thorough incident investigation, mandatory learning from adverse events, and a commitment to openness and transparency with affected families. This includes ensuring that regulatory bodies and internal governance structures within NHS trusts are robust, impartial, and capable of driving meaningful change.

A Decade of Documented Failures: The Case of Orlando Davis
The interim review’s findings resonate with a decade of investigative journalism and advocacy by families affected by poor maternity care across numerous NHS trusts in England. High-profile cases at Morecambe Bay, Shrewsbury & Telford, East Kent, Nottingham, and Leeds have consistently revealed patterns of negligence, cover-ups, and systemic failures, indicating that the problems are neither new nor isolated.
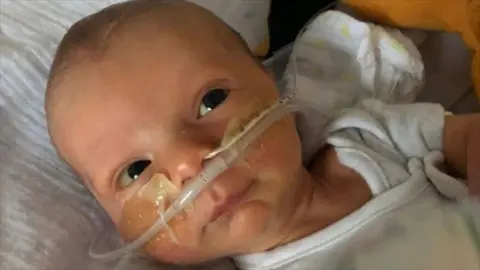
The tragic case of Orlando Davis serves as a stark illustration of the devastating consequences of these systemic issues. Orlando died in September 2021, a mere 14 days after his birth at Worthing Hospital in Sussex. An inquest subsequently concluded that neglect had contributed to his death, specifically citing the failure of staff to detect his mother, Robyn, had developed hyponatremia – a dangerously low level of sodium in the bloodstream – during labour. Robyn and her husband Jonathan firmly believe that the core issue was a fundamental failure to heed her concerns during this critical period. Jonathan described a "cultural" problem within maternity services, where the professional perspective of healthcare providers can overshadow, and ultimately dismiss, the unique knowledge and experience of the mother regarding her own body.
The Davis family is a vocal part of "Truth for Our Babies," a group advocating for a comprehensive, independent investigation into maternity services at the University Hospitals Sussex NHS Trust. Recent reports by BBC News and the New Statesman indicate that at least 55 infant deaths over a five-year span within this Trust could potentially have been averted with improved care. The anguish and loss experienced by families like the Davises underscore the profound human cost of these systemic failures.

Calls for a Statutory Inquiry and Enhanced Oversight
Despite the significance of Baroness Amos’s review, a growing chorus of voices, including the Davis family, argues that its scope may be insufficient to instigate the fundamental change required. They advocate for a statutory inquiry, arguing that it offers a more robust and far-reaching mechanism for accountability compared to the current government-commissioned review. A statutory inquiry, typically established under specific legal powers, possesses the authority to compel witnesses and demand documentation, offering a deeper and more exhaustive investigation into systemic failings, including the performance of regulatory bodies which are currently outside the purview of the Amos review.
Robyn Davis articulated this sentiment, stating that the current review "is not going deep enough" and fails to scrutinize the regulators themselves. Jonathan Davis emphasized the need for "gold standard accountability" for families who have received "lacklustre care," contending that a "rushed, high-level review" falls short of this standard. They believe that a properly conducted statutory inquiry is essential to prevent future mothers and children from suffering similar "irreversible fate."
Complementing this call for a more rigorous investigation, Labour MP Michelle Welsh, a prominent campaigner for maternity safety, has urged the government to implement "big, bold policies" and to establish a dedicated maternity commissioner. Such a commissioner would be responsible for overseeing and driving improvements in maternity care across the country, ensuring consistent standards and advocating for necessary investment and reforms. The delay in establishing the Health Secretary’s promised maternity taskforce, announced last June to spearhead improvements, further fuels concerns about the government’s commitment to decisive action. While the Department for Health and Social Care has stated that membership would be announced "shortly," this protracted delay risks undermining the urgency and momentum needed to address these critical issues.
Conclusion: The Imperative for Transformative Change
The interim report from Baroness Amos’s review serves as a sobering indictment of England’s maternity services, confirming what many families and campaigners have long known: the system is failing. The interwoven issues of racism, chronic understaffing, and a pervasive lack of accountability create a perilous landscape for expectant mothers and their newborns. While the commitment to act on the final recommendations is a positive step, the depth and persistence of these problems demand more than incremental adjustments.
Transformative change requires not only significant financial investment in workforce and infrastructure but also a profound cultural shift within healthcare institutions. This includes dismantling systemic racism, fostering environments where patient concerns are genuinely heard and acted upon, and establishing unequivocal accountability at all levels. Without a comprehensive and unflinching approach that addresses the root causes of these failures, the aspiration for universally safe and excellent maternity care in England will remain an elusive goal, continuing to inflict preventable trauma and loss on countless families. The forthcoming final report and the government’s subsequent response will be a critical juncture in determining the future trajectory of maternity care in the nation.