A significant and rapidly expanding outbreak of measles, a highly contagious viral disease, has gripped several educational institutions across North London, resulting in dozens of confirmed infections among children and raising serious concerns among health authorities. This concerning development underscores the critical need for robust immunisation programmes and highlights the vulnerabilities created by sub-optimal vaccine uptake rates across the region.
Reports from public health bodies confirm a substantial increase in measles cases, particularly concentrated within the boroughs of Enfield and Haringey. Official figures for January alone indicated 34 laboratory-verified infections in Enfield, signaling a swift proliferation of the virus within school and nursery environments. Healthcare providers, including the NHS Ordnance Unity Centre For Health, have issued stark warnings about the speed of transmission and the potential for severe health outcomes, particularly among those without adequate immunological protection.
The clinical ramifications of this outbreak are already evident, with a notable proportion of affected children requiring hospitalisation. Local medical practitioners have observed that approximately one in five pediatric patients diagnosed with measles have necessitated inpatient care, a critical detail often linked directly to their incomplete immunisation status. This statistic serves as a potent reminder of measles’ capacity to cause serious complications, which can range from pneumonia and ear infections to more severe neurological damage and, in rare instances, mortality. The susceptibility of unvaccinated individuals not only jeopardises their own health but also poses a considerable risk to vulnerable populations, such as infants too young for vaccination or individuals with compromised immune systems.
In response to the escalating situation, a concerted public health effort is underway, involving the UK Health Security Agency (UKHSA), Enfield Council, and various local healthcare partners. These collaborative initiatives aim to contain the spread, provide medical support, and intensify public awareness campaigns. Councillor Alev Cazimoglu of Enfield has emphasised the gravity of the situation, noting the need for "additional care with a short stay in hospital" for some affected children. Both local and national health officials are issuing urgent appeals to families to verify and update their children’s vaccination records, advocating for the measles, mumps, and rubella (MMR) vaccine as the most effective preventative measure.
Dr. Vanessa Saliba, a leading expert from the UKHSA, has characterised the current surge as a "big" outbreak predominantly impacting unvaccinated children under the age of ten in educational settings. Her statements reinforce the preventable nature of measles, asserting that two doses of the MMR vaccine provide robust protection against this debilitating illness. She strongly advises parents of children with missed doses to arrange catch-up vaccinations without delay, stressing the collective responsibility to safeguard the wider community, especially those unable to receive the vaccine due to age or medical conditions. Furthermore, with the impending Easter holiday period, Dr. Saliba has cautioned international travellers to verify their immunisation status, given the prevalence of measles in several countries with close ties to the UK and ongoing outbreaks across parts of Europe.
This resurgence of measles in North London is not an isolated incident but rather a localised manifestation of a broader, more concerning trend observed across the UK and globally. Over recent years, there has been a discernible decline in the uptake of the MMR vaccine, contributing directly to the erosion of herd immunity. UKHSA data for 2024-25 reveals that only 84.4% of children nationwide received two doses of the MMR vaccine by their fifth birthday, falling significantly short of the 95% threshold recommended by the World Health Organization (WHO) to effectively prevent widespread outbreaks. This figure marks a steady decline from a peak of 88.8% recorded in 2014-15, signaling a decade-long trajectory of diminishing vaccine coverage.
The implications of this decline are profound. Historically, measles was a common childhood illness, responsible for widespread morbidity and mortality before the introduction of the vaccine. Successful vaccination programmes led to its near eradication in many developed nations, culminating in the UK being declared measles-free by the WHO in 2017. However, the consistent drop in vaccination rates has tragically reversed this progress, leading to the UK losing its measles elimination status in January 2024 following a series of widespread outbreaks. This loss is a stark indicator of the fragility of public health achievements when vaccination rates fall below critical thresholds.
Several factors contribute to the diminished vaccine uptake. Misinformation and disinformation campaigns, often propagated online, have fueled vaccine hesitancy among some segments of the population. Concerns, largely unfounded and repeatedly disproven by scientific consensus, regarding vaccine safety have deterred parents from vaccinating their children. Additionally, issues of access to healthcare services, particularly in post-pandemic environments where routine appointments may have been delayed or missed, have played a role. Complacency, stemming from the historical rarity of measles due to successful vaccination, has also led some to underestimate the severity of the disease and the importance of immunisation.
Measles, caused by the rubeola virus, is among the most infectious human diseases. It spreads via airborne droplets when an infected person coughs or sneezes, capable of lingering in the air for up to two hours after an infected person has left a room. An unvaccinated individual has a 90% chance of contracting measles if exposed to the virus. The incubation period typically lasts 10-12 days before symptoms appear. Initial symptoms, known as the prodromal phase, include a high fever, persistent cough, runny nose (coryza), and red, watery eyes (conjunctivitis). A characteristic diagnostic sign, Koplik spots – small white spots with bluish-white centres on a red background – often appear inside the mouth a few days before the rash.
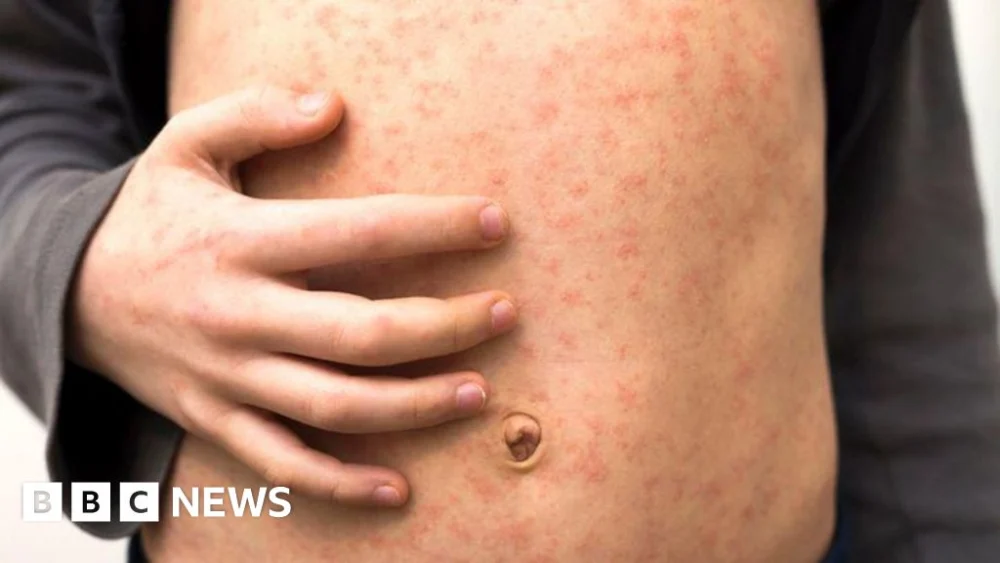
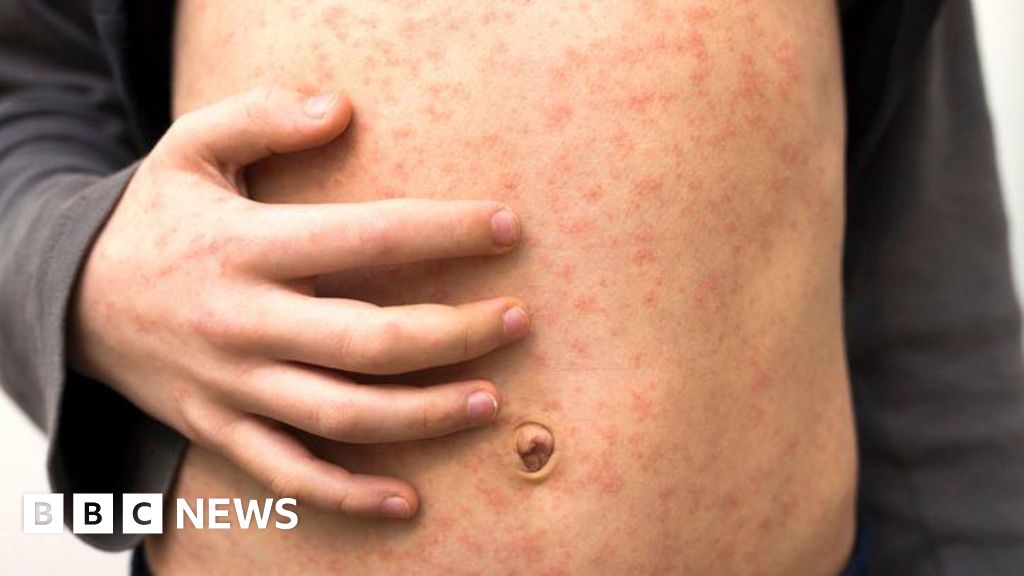
The distinctive blotchy red or brown rash typically emerges three to five days after the initial symptoms, usually starting behind the ears and on the face before spreading downwards to the chest, back, and limbs. On brown and black skin, the rash may be harder to detect, appearing as subtle changes in texture or deeper hues rather than vivid redness, which can complicate early diagnosis. The rash usually lasts for about a week before fading. However, measles is far more than just a rash; it can lead to severe complications. Common secondary infections include ear infections and diarrhoea, but more serious issues like pneumonia (the leading cause of measles-related deaths in young children) and encephalitis (inflammation of the brain) can occur. Subacute sclerosing panencephalitis (SSPE), a rare but fatal degenerative neurological disease, can develop years after a measles infection, even if the child appeared to have fully recovered.
The socio-economic implications of widespread measles outbreaks extend beyond individual health. The strain on healthcare systems is considerable, with pediatric wards and emergency departments facing increased pressure from hospitalised cases. Educational institutions experience disruption due to absenteeism, affecting learning outcomes and potentially requiring school closures to curb transmission. Economically, there are direct costs associated with treatment and public health interventions, as well as indirect costs from lost parental workdays and long-term care for individuals with severe complications. Furthermore, a decline in vaccination rates and the subsequent resurgence of preventable diseases can erode public trust in health authorities and scientific guidance.
Looking forward, addressing this public health challenge requires a multi-faceted approach. Sustained and well-funded catch-up vaccination campaigns are essential to reach individuals who have missed their routine MMR doses. These campaigns must be coupled with enhanced public awareness initiatives that effectively communicate the risks of measles and the proven safety and efficacy of the vaccine, countering misinformation with clear, evidence-based information. Healthcare providers play a crucial role in advocating for vaccination and addressing parental concerns. Robust disease surveillance and contact tracing mechanisms are vital for early detection and rapid response to contain future outbreaks. Policy considerations may also need to be reviewed, potentially including more stringent school entry vaccination requirements or targeted outreach programmes for communities with historically low uptake. Globally, the interconnectedness of societies means that maintaining high vaccination rates everywhere is crucial to preventing the reintroduction and spread of infectious diseases across borders.
In conclusion, the current measles outbreak in North London serves as a critical warning. It underscores the fragility of collective immunity when vaccination rates falter and highlights the immediate and severe consequences for affected children and the wider community. The imperative for universal, timely vaccination against measles is unequivocal, not only to protect individual health but to safeguard public health achievements and prevent further suffering from a preventable disease.







