A landmark preliminary study has cast new light on Cerebral Amyloid Angiopathy (CAA), a pervasive yet often silent brain disorder, revealing that individuals diagnosed with this condition face a profoundly elevated risk of developing dementia, potentially quadrupling their susceptibility within a five-year timeframe, even in the absence of a prior stroke incident. These critical findings, which underscore the urgent need for heightened awareness and proactive clinical management, are slated for presentation at the American Stroke Association’s International Stroke Conference 2026, a preeminent global forum for advancements in stroke research and neurological health, scheduled to convene in New Orleans from February 4-6, 2026.
The Intricate Pathology of Cerebral Amyloid Angiopathy
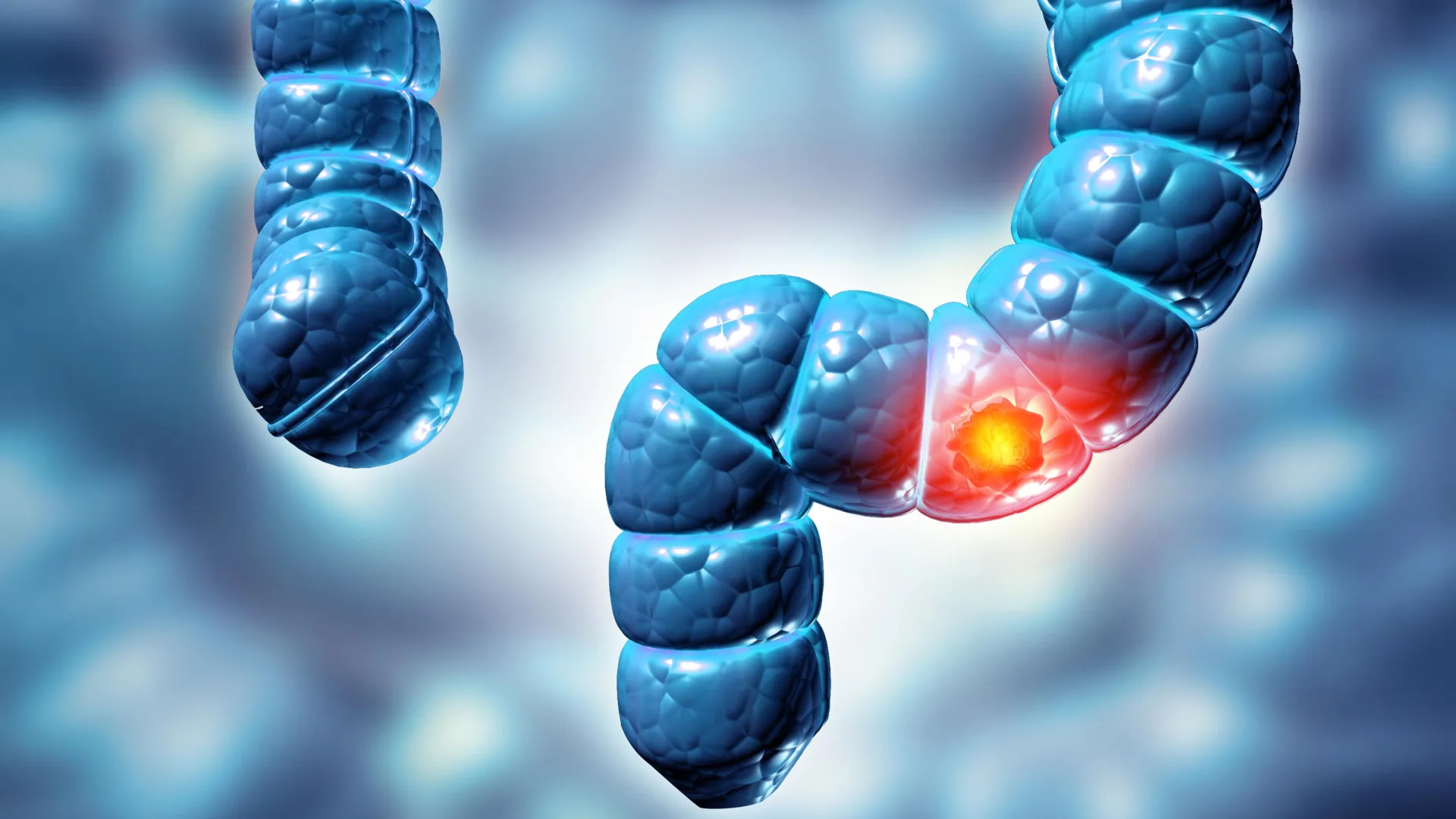
Cerebral Amyloid Angiopathy represents a progressive cerebrovascular disorder characterized by the insidious accumulation of amyloid-beta protein within the walls of small to medium-sized arteries, arterioles, and capillaries of the cerebral cortex and leptomeninges. This pathological deposition gradually compromises the structural integrity and functionality of these vital blood vessels, rendering them fragile and prone to rupture or occlusion. Unlike the amyloid plaques observed in the brain parenchyma of Alzheimer’s disease patients, CAA specifically targets the vascular system, though both conditions frequently co-exist, suggesting a shared underlying pathophysiology or synergistic destructive pathways.
The initial stages of amyloid deposition may occur without overt clinical symptoms, often detected incidentally during neuropathological examination. However, as the amyloid burden intensifies, it precipitates a cascade of detrimental effects. The protein buildup leads to vessel wall thickening, a phenomenon known as "fibrinoid necrosis," and impairs the normal elasticity and reactivity of these vessels. This progressive damage culminates in several severe neurological manifestations. Foremost among these is an increased propensity for hemorrhagic stroke, also known as intracerebral hemorrhage, where weakened vessel walls crack, allowing blood to leak into surrounding brain tissue. Furthermore, CAA significantly elevates the risk of ischemic stroke, which occurs when blood clots obstruct blood flow to parts of the brain. Beyond these acute cerebrovascular events, CAA is increasingly recognized as a major contributor to cognitive decline and dementia, even in the absence of macroscopic strokes, pointing to more subtle, chronic mechanisms of brain injury.
Unraveling the Dementia Link: A Critical Research Imperative
Despite the growing recognition of CAA’s role in cerebrovascular disease and cognitive impairment, comprehensive, large-scale data quantifying the specific trajectory and speed of dementia progression following a CAA diagnosis has remained elusive for clinicians. This knowledge gap has historically hindered the development of clear prognostic guidelines and targeted intervention strategies for affected patients. Addressing this critical need was the primary impetus behind the extensive Medicare study.
Dr. Samuel S. Bruce, M.D., M.A., an assistant professor of neurology at Weill Cornell Medicine in New York City and a lead author of the study, articulated the research team’s objective: "While it is acknowledged that a substantial proportion of individuals with CAA will eventually develop dementia, precise, population-level estimates regarding the frequency and pace of this cognitive decline have not been readily available to guide clinical practice. Our investigation sought to generate robust estimates from a vast cohort of Medicare beneficiaries, specifically examining the likelihood of a new dementia diagnosis in CAA patients and elucidating the distinct and combined influences of CAA and stroke on this risk." The study’s rigorous methodology aimed to disentangle the complex interplay between these neurological conditions and subsequent cognitive deterioration, offering a more granular understanding of their individual and synergistic contributions.
Methodology: A Deep Dive into Medicare Data
To achieve their research objectives, the investigators undertook a comprehensive retrospective analysis of health records from an expansive cohort of more than 1.9 million Medicare beneficiaries aged 65 and older. The dataset spanned a significant period, encompassing the years 2016 through 2022, providing a rich, real-world tapestry of patient health journeys. The research team meticulously reviewed these records to identify new diagnoses of dementia and to scrutinize how both ischemic and hemorrhagic strokes modulated the risk of dementia among individuals previously diagnosed with CAA.
A particularly insightful aspect of the study design involved tracking participants’ health status transitions over time. This dynamic approach allowed researchers to categorize individuals into distinct health states: periods with no CAA or stroke, periods with CAA alone, periods with stroke alone, or periods where both conditions were present. Dr. Bruce elaborated on the significance of this methodology: "By meticulously tracking these transitions, we were able to precisely measure the duration individuals spent in each clinical category and, crucially, pinpoint the exact timing of a first dementia diagnosis. This enabled us to establish temporal relationships and more accurately attribute risk." This detailed longitudinal perspective provided a powerful framework for assessing the independent and interdependent contributions of CAA and stroke to the incidence of dementia.
Profound Revelations: CAA’s Dominant Role in Dementia Risk
The meticulous analysis of the extensive Medicare dataset yielded compelling and clinically significant findings, firmly establishing CAA as a substantial and independent driver of dementia risk within the observed five-year timeframe. The study unequivocally demonstrated that CAA exerts a more potent influence on the likelihood of developing dementia than stroke alone.
The most striking revelation was the finding that individuals with a diagnosis of CAA exhibited approximately four times the risk of developing dementia compared to those without the condition. This dramatic increase in susceptibility underscores CAA’s profound impact on long-term cognitive health. Furthermore, a pivotal discovery highlighted that the risk of progressing to dementia in patients with CAA who had not experienced a stroke was remarkably similar to the risk observed in those with CAA who had suffered a stroke. Both these CAA groups, irrespective of stroke history, exhibited a significantly higher incidence of dementia compared to participants who had experienced a stroke but did not have a CAA diagnosis.
Dr. Bruce emphasized the implications of these findings: "What truly stood out was the comparable dementia risk among those with CAA, whether or not they had experienced a stroke. This risk was consistently higher than in participants who had only experienced a stroke. This strongly suggests that underlying mechanisms unrelated to macroscopic stroke events play a fundamental role in driving dementia risk in CAA patients." These non-stroke-related mechanisms could encompass chronic microbleeds, widespread white matter changes, subtle cerebral hypoperfusion, neuroinflammation, and direct neuronal toxicity resulting from chronic amyloid deposition within vessel walls. The results unequivocally highlight the critical need for proactive screening for cognitive changes following a CAA diagnosis and aggressive management of modifiable risk factors to mitigate further cognitive decline.
Expert Endorsement and Broader Contextualization
The study’s findings resonate strongly within the broader scientific understanding of neurodegenerative disorders, particularly the evolving appreciation for the role of small vessel diseases in the etiology of dementia. Dr. Steven M. Greenberg, M.D., Ph.D., FAHA, a distinguished professor of neurology at Harvard Medical School in Boston, former chair of the International Stroke Conference, and author of influential commentaries on Cerebral Amyloid Angiopathy, provided an independent expert perspective. While not directly involved in the study, Dr. Greenberg affirmed that the results align perfectly with current insights into dementia risk.
"Diseases affecting the brain’s delicate small blood vessels are increasingly recognized as paramount contributors to the global burden of dementia," Dr. Greenberg stated. "This is particularly true for CAA, a condition that frequently co-occurs with Alzheimer’s disease, forming a potent synergistic challenge to brain health. While we have long known about the elevated risk for dementia following any type of stroke, these new results compellingly indicate an even greater and more direct risk specifically for patients diagnosed with CAA, independent of their stroke history." This expert commentary reinforces the study’s significance, positioning CAA not merely as a stroke risk factor but as a direct, independent, and powerful determinant of cognitive decline, often in concert with other neurodegenerative pathologies. The confluence of CAA and Alzheimer’s disease represents a particularly aggressive form of cognitive impairment, necessitating a comprehensive approach to diagnosis and management.
Methodological Caveats and Future Research Imperatives
While the study’s extensive dataset and robust analytical approach provide invaluable insights, the researchers meticulously acknowledged certain inherent limitations. The primary constraint stemmed from the reliance on administrative diagnosis codes derived from inpatient and outpatient Medicare insurance claims, rather than detailed, direct clinical evaluations or neuropathological confirmations. Dr. Bruce noted, "These codes serve as an imperfect proxy for definitive clinical diagnoses, and consequently, misclassifications can occur." To mitigate this potential issue, the research team judiciously employed diagnosis codes that have been previously validated and demonstrated to accurately reflect real-world clinical diagnoses within administrative datasets. Another acknowledged limitation was the absence of imaging data, such as MRI or CT scans, which are considered gold standards for precisely confirming CAA and stroke diagnoses and assessing their severity.
In light of these limitations, the authors underscored the imperative for continued research. They specifically called for prospective studies, which would involve actively following patients forward in time rather than relying on historical records. Such studies would allow for more precise control over diagnostic criteria, more frequent and standardized cognitive assessments, and the collection of multimodal data, including advanced neuroimaging biomarkers. Future investigations should also prioritize the implementation of standardized diagnostic methods for both CAA and stroke, ideally integrating advanced imaging techniques and validated cognitive assessment tools to provide an even more accurate and granular understanding of this complex disease and its trajectory. Furthermore, focused research is needed to unravel the precise non-stroke mechanisms by which CAA contributes to dementia, paving the way for targeted therapeutic interventions.
Study Design and Participant Demographics
This retrospective cohort study meticulously analyzed Medicare claims data for a massive population of 1,909,365 adults residing in the United States. During the specified study period, a total of 752 individuals, representing 0.04% of the overall cohort, received a formal diagnosis of Cerebral Amyloid Angiopathy.
All participants included in the analysis were aged 65 years or older, with a collective average age of 73 years. The study population exhibited a balanced gender distribution, with women constituting 54% and men accounting for 46% of the cohort. Racially, the group comprised 82.4% white adults, 7.3% black adults, and 10.3% individuals from other diverse racial backgrounds. The data utilized for the analysis were extracted from Medicare health insurance claims submitted by clinicians and hospitals during the course of routine patient care, spanning multiple years from 2016 to 2022. This extensive, real-world dataset provides a powerful foundation for the study’s conclusions, reflecting the demographic and clinical realities of the older adult population in the United States.
Conclusion: A Call for Heightened Vigilance
The findings from this large-scale Medicare study represent a significant advance in our understanding of Cerebral Amyloid Angiopathy, firmly establishing it as a profoundly impactful and independent risk factor for the rapid progression to dementia. The fourfold increase in dementia risk, particularly in the absence of overt stroke, signals that CAA’s influence on cognitive decline is more pervasive and direct than previously fully appreciated. This research serves as a clarion call for the medical community to elevate CAA’s prominence in the differential diagnosis of cognitive impairment, especially in older adults. Increased awareness, earlier and more accurate diagnosis through advanced neuroimaging, and the development of targeted therapeutic strategies are now paramount to mitigate the devastating cognitive consequences of this often silent, yet potent, brain disease. As the scientific community converges at the International Stroke Conference 2026, these findings are poised to reshape clinical paradigms and propel future research into effective interventions for CAA-related dementia.